Scientists Uncover Hidden Trigger Behind Stem Cell Aging
A known cell-death protein turns out to quietly reshape stem cell aging.
As people grow older, the body’s ability to maintain healthy blood and a strong immune system gradually weakens. A major reason is the decline of hematopoietic stem cells (HSCs), which are responsible for producing all types of blood cells.
Under normal conditions, HSCs can renew themselves and generate a balanced range of blood cells. With age, however, they become less efficient. They produce fewer new cells, increasingly favor myeloid cells over lymphoid cells, and are less capable of sustaining a strong immune response.
This decline is linked to accumulated cellular damage, changes in gene activity, chronic low-level inflammation, and alterations in the bone marrow environment. Still, how these different stress factors combine to impair HSC function has remained unclear.
Investigating a Nontraditional Aging Pathway
Researchers from the University of Tokyo in Japan and St. Jude Children’s Research Hospital in the United States set out to better understand how age-related stress disrupts HSC function.
They focused on the receptor-interacting protein kinase 3 (RIPK3)-mixed lineage kinase-like (MLKL) signaling pathway, which is typically associated with necroptosis, a form of programmed cell death. The study was led by Dr. Masayuki Yamashita.
Explaining the motivation behind the study, Dr. Yamashita says, “We discovered an unexpected phenotype in HSCs of MLKL-knockout mice repeatedly treated with 5-fluorouracil, where aging-associated functional changes were markedly attenuated despite no detectable difference in HSC death, prompting us to investigate whether this pathway might induce functional changes beyond cell death.”
This finding shifted attention toward a non-lethal role for MLKL, a concept later explored in their study published in the journal Nature Communications.
Experimental Approach and Methods
To examine this idea, the researchers used several types of genetically modified mice, including wild-type, MLKL-deficient, and RIPK3-deficient models. They also used specialized reporter mice that can detect MLKL activation using a Förster resonance energy transfer-based biosensor. The animals were exposed to conditions that mimic aging-related stress, such as inflammation, replication stress, and oncogenic stress.
The team evaluated HSC function mainly through bone marrow transplantation, a method that measures how effectively stem cells can rebuild the blood system. Additional techniques included flow cytometry, ex vivo expansion, RNA sequencing, assay for transposase-accessible chromatin sequencing, high-resolution microscopy, metabolic testing, and mitochondrial analysis. These methods allowed researchers to examine how MLKL activity affects HSCs at multiple biological levels.
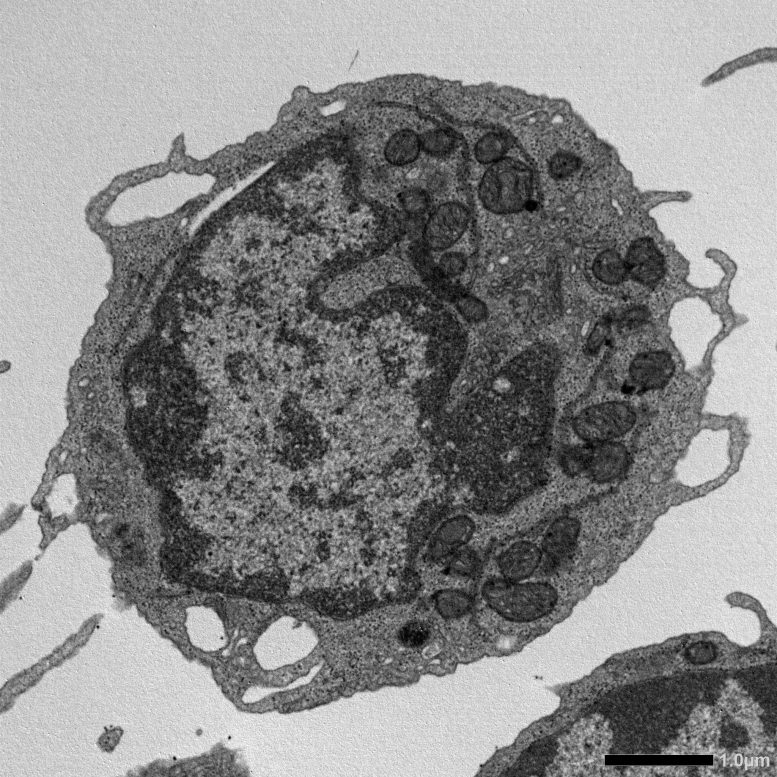
The findings revealed an unexpected role for MLKL that does not involve cell death. Although MLKL is usually linked to necroptosis, its activation in HSCs did not increase cell death or reduce cell numbers. Instead, stress triggered a temporary activation of MLKL within mitochondria. This led to direct mitochondrial damage, including reduced membrane potential, structural changes, and impaired energy production. As a result, HSCs developed key features of aging, such as reduced self-renewal, decreased lymphoid cell production, and a shift toward myeloid cell output.
Protective Effects of MLKL Inactivation
Disabling or removing MLKL significantly reduced these harmful effects. HSCs lacking MLKL retained their ability to regenerate, produced more balanced immune cells, showed lower levels of DNA damage, and maintained healthier mitochondrial function, even under stress or in older animals.
Notably, these benefits occurred without major changes in gene expression or chromatin accessibility. This suggests that MLKL contributes to HSC aging through mechanisms that act after gene transcription and at the level of cellular structures, rather than through changes in gene regulation or inflammation.
These results offer new insight into how aging affects the blood system and point to potential therapeutic strategies. By connecting multiple stress signals to mitochondrial damage through MLKL, the study identifies a shared pathway that may drive HSC decline.
Dr. Yamashita emphasizes, “In the longer term, this research could lead to therapies that preserve the function of hematopoietic stem cells, ultimately improving recovery and long-term health for patients undergoing chemotherapy, radiation, or transplantation. By revealing how non-lethal activation of cell-death pathways drives stem cell aging, these findings may inspire new classes of mitochondrial-protective or necroptosis-modulating drugs.”
Redefining the Role of MLKL
Overall, the study reveals that MLKL plays an unexpected role in stem cell aging. Rather than causing cell death, it responds to stress by damaging mitochondria and weakening HSC function.
These findings reshape our understanding of necroptosis-related proteins and highlight new possibilities for slowing or preventing age-related decline in the hematopoietic system.
Source: SciTechDaily
Scientists Can Now Read Your Body Clock From a Single Hair
Scientists Uncover Hidden Trigger Behind Stem Cell Aging